Hypothermia
Hypothermia is defined as core temperature (measured by oesophageal, rectal or bladder probe) of < 35°C.
Predisposing factors
Increased loss:
- exposure/entrapment
- cold water immersion
- vasodilation, such as by alcohol, drugs/medications and sepsis
- Skin conditions, such as psoriasis, burns, erythoderma and TEN.
Decreased production:
- Age – neonates, elderly
- Endocrine failure – pituitary, thyroid or adrenal insufficiency
- Nutritional deficiency – hypoglycaemia, anorexia, malnutrition
- Inactivity, immobility
- Muscle relaxants
CNS dysfunction:
- Drugs – sedatives, alcohol, opioids
- CNS – trauma, intracranial haemorrhage, neoplasm
- Acidosis, anoxia or encephalopathy
Presentation
It can be further categorised:

Mild (35-32°C)
Moderate (32-28°C)
Severe (<28°C)
Mild hypothermia (32-35°C)
- Associated with increased basal metabolic rate
- Maximal shivering (for thermogenesis)
- Amnesia, dysarthria, ataxia, apathy
- Normal blood pressure.
Moderate hypothermia (28-32°C)
- Progressive reduction in temperature results in stupor
- Shivering stops
- Atrial fibrillation and other dysrhythmias develop, cardiac output 2/3 of normal
- Progressive loss of consciousness, pulse and respiration; pupils dilated at 29°C.
Severe hypothermia (< 28°C)
- Loss of reflexes and progressive paralysis - reflexes absent at 26°C
- Major acid base disturbance
- Significant reduction in cerebral blood flow (1/3) and cardiac output (45%) at 25°C
- Pulmonary oedema, significant hypotension and bradycardia develop
- Maximum risk of VF at 22°C
- Flat EEG at 19°C, asystole at 18°C
Investigations
Bedside:
- Temperature measurement, rectal, oesophageal, bladder temperature probe
- BSL
- ECG
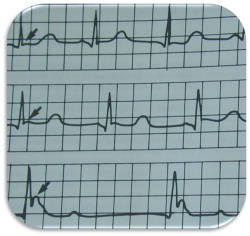
bradycardia, atrial fibrillation (AF)
prolonged PR, QRS and QT intervals
"J” or Osborne waves - “J” gets bigger the more severe the hypothermia
ST junction elevation due to delayed depolarisation with temp
Laboratory
- FBC - WCC in sepsis
- EUC, Hypo- or hyperkalaemia
- Acute renal failure (high urea and creatinine)
- BSL, Hypo- or hyperglycaemia
- Clotting studies, Coagulopathy and DIC
- Venous blood gases (VBG)
- mild often shows a respiratory alkalosis
- moderate to severe progresses to a mixed metabolic and respiratory acidosis
Management
- Primary survey, ABCDE approach and immediate resuscitation in systems, including oxygen, IV analgesia and (warmed 42°C) fluids via x2 large bore cannulae
- Measure pulse for 1 minute, commence CPR
- Call for help early - senior ED
- remove wet clothing, towels, blankets
- gentle handling of patient (rough handling may precipitate cardiac dysrhythmias – probably overstated)
- consider traumatic or medical causes for hypothermia
- correct dehydration with warmed IV fluids
- correct hypoglycaemia with IV dextrose
- cover with warm blankets or heated air blankets (“Bair Hugger”)
- temperature should increase in a warm room with the above measures (approx 2°C per hour)
Rewarming Techniques
Passive rewarming
- Usually sufficient for mild hypothermia
- Involves removal of wet clothing, keep patient in warm, dry environment with blankets
Active external rewarming
- Indicated for moderate hypothermia
- External application of heat via heated air blankets (“Bair hugger”) and radiant heat
Active internal rewarming
- Warmed humidified oxygen at 40-45°C (if not available in the ED may be available in operating theatres or ICU)
- Blood / fluid warmer for all IV infusions
- Warm water lavage via
- thoracic closed lavage (constant flow using 2 tubes possible), or left sided thoracotomy
- urinary catheter
- peritoneal
- (nasogastric, rectal tube, less effective, more risk, use other places first)
- Cardiopulmonary bypass (CPB) or ECMO if available has also been used for life-threatening cases (severe hypothermia)
If CPB not available pleural lavage can be used with warm water/saline
Cardiac Management Issues
Cardiac Dysrhythmias:
- CPR for asystole and VF
- VF may not be successfully electrically cardioverted until the temperature is >30°C
- AF will revert spontaneously when the temperature returns towards normal, bradycardia is a normal physiological response to hypothermia and needs no treatment
Management - Cardiac Arrest:
- Hypothermia is neuro (brain) protective
- Don’t diagnose death in a cold patient - wait until they are “warm (>30°C) and dead”
- CPR as standard 30:2 ratio
- Active core rewarming techniques, used during CPR
- Drugs and cardioversion unlikely to be effective until the temperature rises to >30°C
- Double the time between drug doses during CPR at temps between 30°C and 35°C
Further Reference and Resources
- First Aid Management of Hypothermia and Cold-Related Injuries (Guideline 9.3.3) - Australian Resuscitation Council
- Brown, DA, Brugger, H, et al. (2012) Accidental hypothermia NEJM; 367: pp.1930-8